Riding the open road comes with risks. How do motorcycle helmets reduce them, and by how much?
There’s nothing like riding a motorcycle; senses alight as the wind whips your body, and reflexes become one with the machine. But every rider knows that the pleasures, including head-snapping acceleration on-demand, come with more risk than driving a larger vehicle. Motorcycle injuries, especially head injuries, must be considered and prevented to the extent possible.
Here’s a look at the real risks of motorcycle accidents, with a focus on head trauma and the protective impact of helmets.
A review of motorcycle accident injuries and fatalities
Deaths
Motorcycles are fast, less visible to other drivers, and obviously offer far less protection than bigger vehicles, which is why the National Highway Traffic Safety Administration (NHTSA) estimates “the number of deaths on motorcycles [is] nearly 24 times the number in cars” per mile traveled.
For example, there have been over 42,000 overall US motor vehicle deaths in each of the past two years of available data. This annual number has varied from a low of 32,479 (2011) to a high of 42,939 (2021) in the past 15 years.
Motorcycle accident deaths represented 14% of fatalities in both of those years (4,630 in 2011 and 6,084 in 2021), ranging from 13% to 15% over a 15-year period. The proportions are high, considering motorcycles are only about 3% of registered vehicles.

Injury stats and types
Stats on injuries from motorcycle accidents tell a somewhat different story, however. While total bike deaths have increased by 20% between 2010 and 2020, injuries have remained essentially flat — “just a 1% rise” overall. The highest number of riders injured in that period was 104,442 in 2016, and the lowest was 81,706 in 2011.
Injuries among riders are broken down into various categories:
- Head, face, or neck injuries
- Road rash, where sliding against the ground peels away soft tissue
- Arm, aka “upper extremity” injuries, often due to bracing against impact
- Leg, aka “lower extremity” injuries, whether it’s from friction or the bike falling on legs
- Trunk, aka “thorax,” and abdominal injuries
There aren’t definitive stats on how often each injury type occurs, but various research attempts to nail down the number. For example, a study of 4,200 patients seen over two years in an Iranian trauma center revealed the following patterns:
- “The head was the most commonly injured site of the body, followed by the foot, face, and forearm.”
- Upper limb trauma was observed in 78.8% of patients
- Lower limb trauma: 60.9%
- “67.1% … had traumas in more than two regions of the body”
- “59.7% of the admitted patients and 85.4% of total death cases had head injuries”
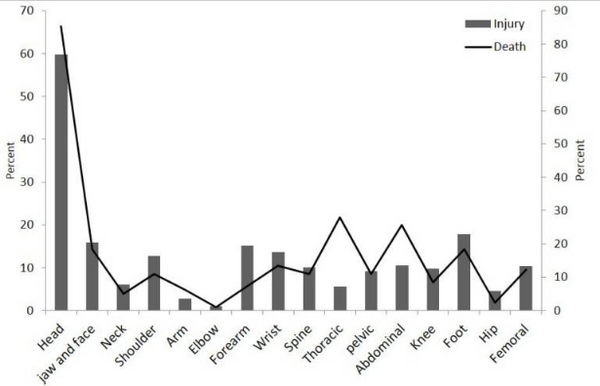
Head injuries were the largest share of injuries seen in these motorcycle accident patients seen at a trauma center over two years. Source: Sayyed Hoseinian SH, Ebrahimzadeh MH, Peivandi MT, et al. Injury Patterns among Motorcyclist Trauma Patients: A Cross Sectional Study on 4200 Patients. Arch Bone Jt Surg. 2019.
Another review looked at all hospitalized motorcyclists in Maryland between 1998 and 2002, comparing injuries by age (above and below 40). This research found results that seem very different, with studied groups having way more harm to the extremities than the head.
However, some of that difference is in how the next researchers categorized things—they didn’t individually break out arm, elbow, forearm, and wrist injuries within “upper extremity” wounds, for example:
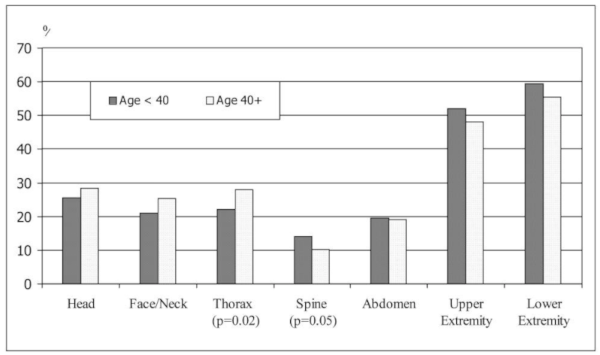
"Distribution of Injured Anatomic Region by Age Group." Source: Dischinger PC, Ryb GE, Ho SM, Braver ER. Injury patterns and severity among hospitalized motorcyclists: a comparison of younger and older riders. Annu Proc Assoc Adv Automot Med. 2006;50:237-249.
NHSTA data from 2003–2005 generally supports these break downs. The agency reports that a “majority of hospitalized motorcyclists’ injuries were to the upper and lower extremities” while “more than 15 percent of motorcyclists sustained head injuries.”
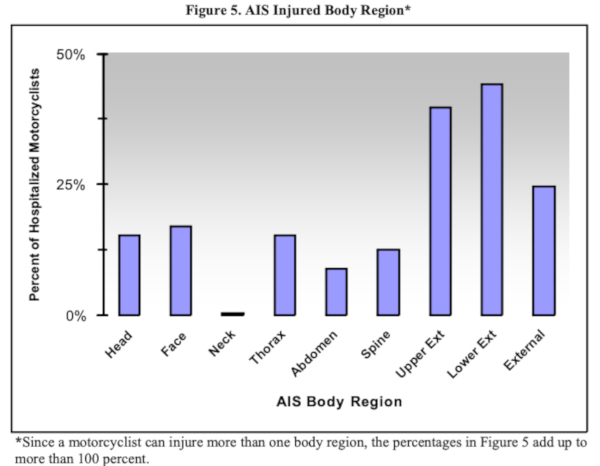
Source: "Motorcycle Helmet Use and Head and Facial Injuries." NHTSA
Head injuries from motorcycle accidents: types and effects
Head injuries present outsized risks to riders and passengers, causing about 37% of all motorcycle crash fatalities. Here’s how the types of traumatic head and brain injuries break down:
- Impact loading is “a blow directed through the center of mass of the head”— basically, a direct hit into/by an object.
- Impulse loading is “when an oblique impact … creates tangential forces, causing head rotation.” In addition to potentially harming the neck, the brain moves within the skull, putting “mechanical strain on cerebral blood vessels, nerve fibers and brain tissue.” This often happens due to “sudden deceleration when the rider’s body hits the road after being thrown off of his or her vehicle.”
Head injuries are further divided into:
- Closed: the skull remains intact, but the person can suffer lacerations and contusions (bruises), potentially resulting in traumatic brain injury (TBI). Closed head injuries can vary from mild to severe.
- Open: an object penetrates and fractures the skull, damaging the brain and surrounding tissue.
Impulse-loading injuries are closed, while impact-loading injuries may be open or closed. The effects of various head wounds may include:
- Subdural hemorrhages (internal bleeding between the brain and skull)
- Diffuse axonal injury (DAI): brain tissue tears from inertia
- Concussions and other TBIs
- Lacerations and bruising of the head and underlying brain tissue
The damage and risks of open head injuries are more obvious, whereas closed injuries may have subtle effects that also persist — and they require dedicated scans and close observation.
For example, one study of 184 riders with head injuries found that 31.6% of patients who failed to receive a CT scan died, whereas 95.5% of those with “normal findings on brain CT scan survived.” The authors’ conclusion: “Computed tomography scan represents an indispensable, lifesaving diagnostic tool.”
And surviving a head injury isn’t the end of the story, as individuals may suffer from loss of concentration, debilitating headaches, and other chronic symptoms and conditions. Here’s one sobering data point:
According to one study, the employment rate before sustaining a moderate or severe TBI was 80%, but the rate was just 15% three months after injury, and the rate had only increased to 55% three years following injury.
It’s easy to see why preventing severe head injuries from motorcycle accidents is crucial—and why 47 US states have partial or universal helmet laws.
CT scans are an essential diagnostic tool for accurately assessing motorcycle accident head injuries.
Motorcycle injuries and fatalities: no helmet vs. helmet
Helmets significantly reduce severe injuries and deaths. About 60% of riders who die wear them, but a Government Accountability Office (GAO) review of 46 safety studies reports the total deaths and serious injuries would be much higher without headgear.
- “Helmeted riders have up to a 73 percent lower fatality rate than unhelmeted riders.”
- “Helmeted riders have up to an 85 percent reduced incidence of severe, serious, and critical injuries than unhelmeted riders.”
National Highway Traffic Safety Administration (NHTSA) stats offer similar conclusions:
- “Motorcycle helmets are 67 percent effective in preventing brain injuries.”
- “Unhelmeted motorcyclists are over three times as likely to suffer a brain injury as were those who were helmeted.”
Motorcycle helmets vary in design but protect the rider with three elements:
- An outer shell that protects against penetrating objects and distributes the force of impact over a more extensive, strong surface area.
- A liner that surrounds the head further reduces the impact force and head velocity.
- A retention system that keeps the helmet in place. The most common is a strap with a Double-D-ring design.
The combination of a shell and liner distributing the energy of an impact and slowing head acceleration can lessen both impact- and impulse-loading injuries. And this protective headgear is particularly good at stopping penetrations.
However, motorcycle helmets have their limits, particularly when it comes to preventing TBIs. In addition, ultimately, the severity of any injury depends on the speed of impact. Dr. John Lloyd, a leading motorcycle accident expert, offered these conclusions in a study testing 10 popular motorcycle helmets:
The purpose of a motorcycle helmet is to reduce blunt force trauma to the head, thereby decreasing the risk of lacerations, contusions and skull fractures. [...] [H]elmets can and do prevent fatalities associated with penetrating head trauma. […] However, as with most helmets, motorcycle helmets perform inadequately in terms of mitigating the forces responsible for causing traumatic brain injury.
A review published in Injury Epidemiology echoes his conclusions. Researchers analyzed and compared data from five US states that universally mandate helmets against six states with partial laws, where headgear is optional if riders meet specific criteria.
The results show how higher helmet usage in universal law states (88% vs. 42%) mitigated all injury types but had a less dramatic but still positive effect on reducing TBIs (the bottom left quadrant below):
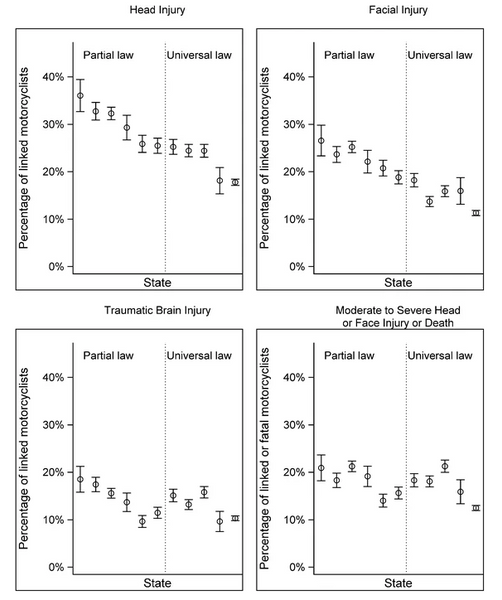
Source: Olsen, C.S., Thomas, A.M., Singleton, M. et al. Motorcycle helmet effectiveness in reducing head, face and brain injuries by state and helmet law. Inj. Epidemiol. 3, 8 (2016). (CC BY 4.0 DEED)
Nevertheless, despite these limitations, helmets save many lives and significantly prevent or lessen motorcycle head injuries.
As the researchers in the above review concluded: “Medical outcomes […] were more severe among injured motorcyclists in partial law states. Motorcyclists in partial law states were more likely to sustain head, facial, and traumatic brain injuries compared to those in universal law states.”
Further, an “enormous amount of research has shown and quantified the effectiveness of motorcycle helmets in reducing morbidity and mortality.”

Helmets mitigate motorcycle accident injuries — but safety goes beyond protective gear
Depending on the laws in your state, the decision to wear a helmet—and what type—can be a personal one. Some individuals state comfort, visibility, and a feeling of freedom as reasons for not using protective headgear. Others wouldn’t even consider riding without helmets.
Regardless, the joy of riding a motorcycle comes with elevated risks compared to other vehicles, and helmets are incredibly valuable for lowering the odds of severe injury or death. Wearing a helmet is absolutely recommended. However, safely operating a motorcycle—remaining aware and vigilant and especially watching one’s speed in risky situations—is arguably more vital.
Check out the rest of the Hard Head Veterans blog to learn more about head injuries and helmets, including how helmets mitigate TBIs and other wounds.
